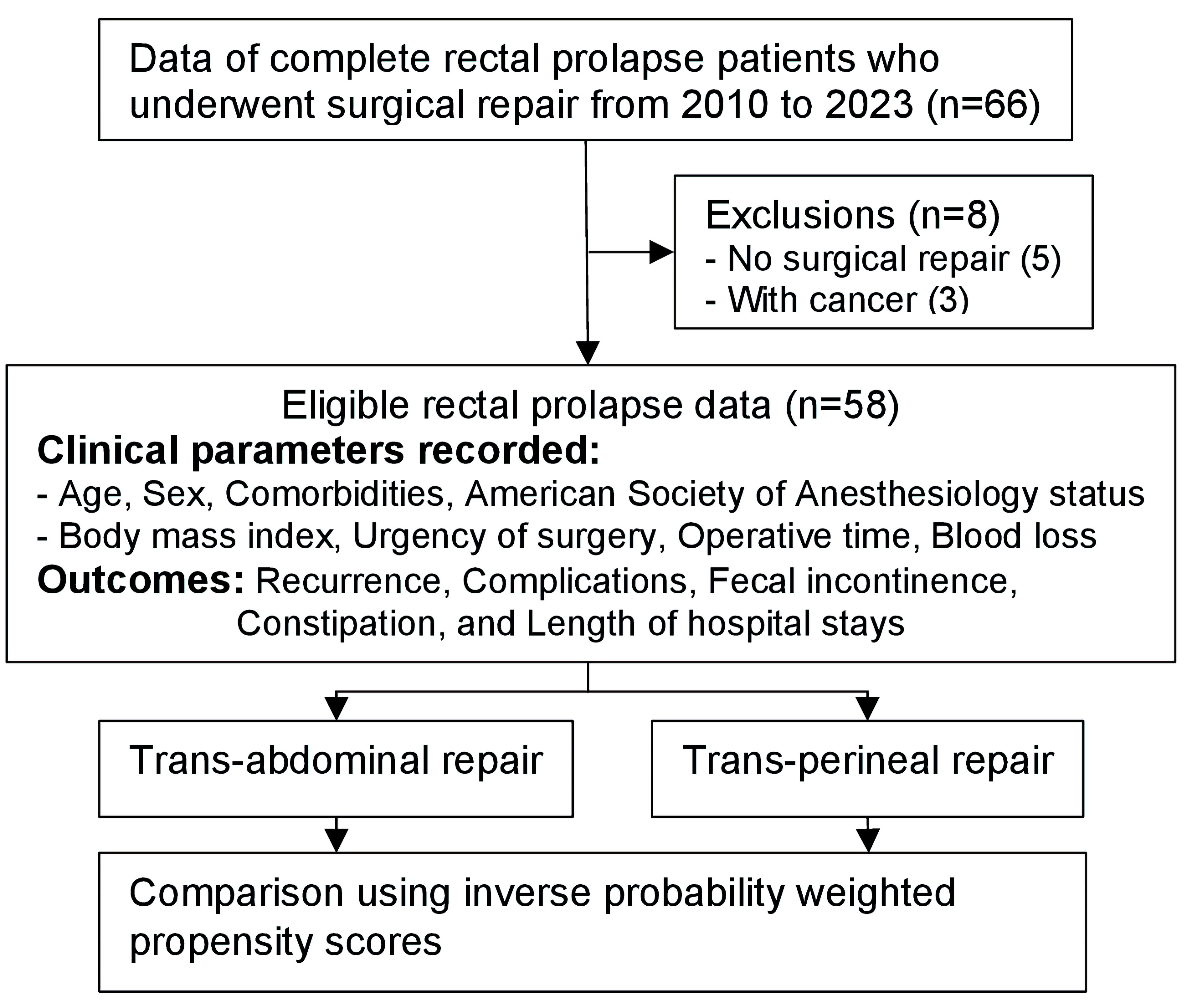
↓ Figure 1. The study participants’ flow.
| Gastroenterology Research, ISSN 1918-2805 print, 1918-2813 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, Gastroenterol Res and Elmer Press Inc |
| Journal website https://gr.elmerpub.com |
Original Article
Volume 18, Number 2, April 2025, pages 85-92
Comparative Outcomes of Transabdominal and Transperineal Approaches for Full-Thickness Rectal Prolapse Repair: A Fourteen-Year Retrospective Study
Figures

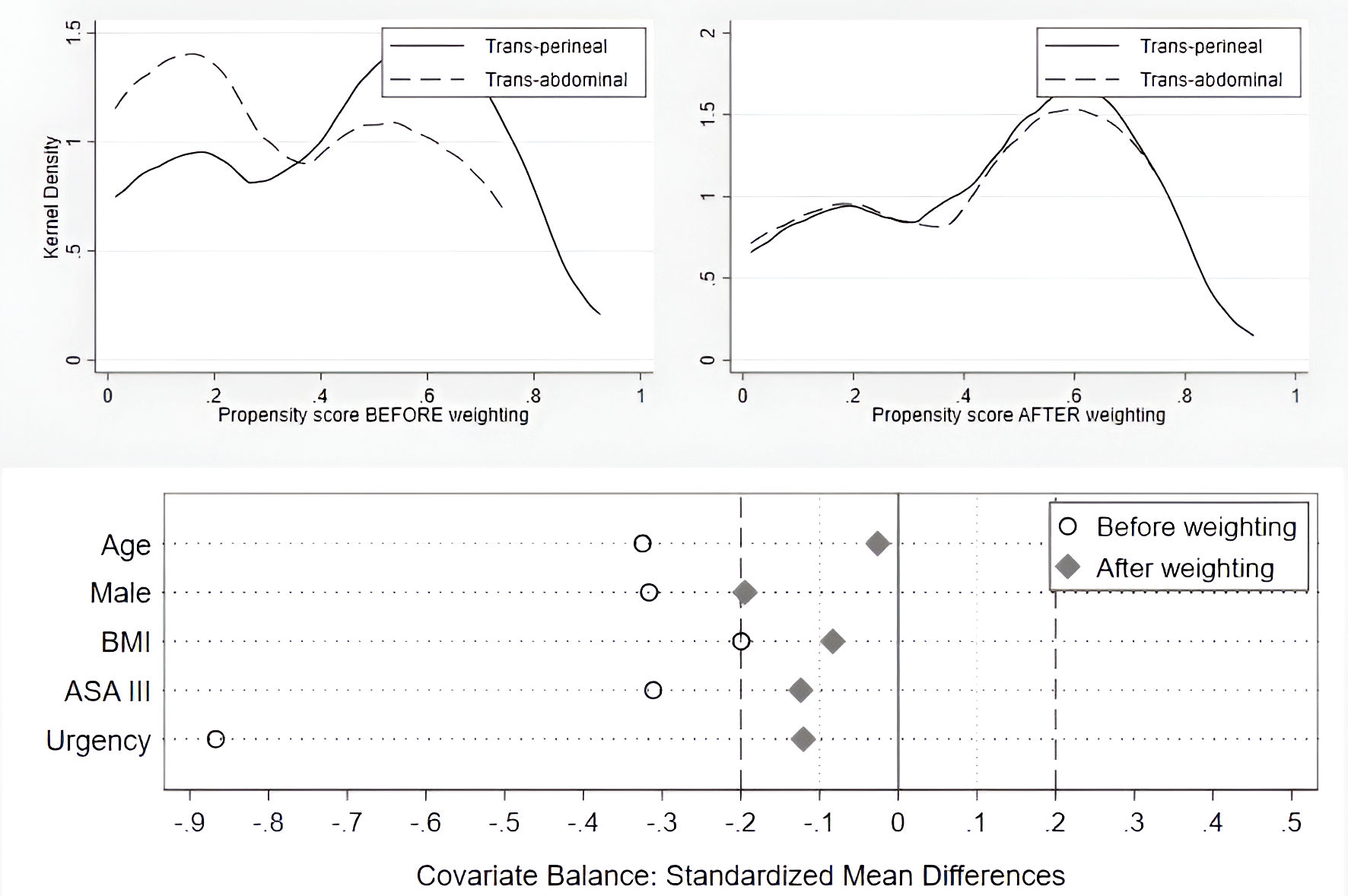
Tables
| Variable, n (%) | Transperineal (n = 33) | Transabdominal (n = 25) | P value |
|---|---|---|---|
| aMultimorbidity is defined as patients having two or more comorbidities or being bedridden. bNumbers of patients were 24 (transperineal) vs. 23 (transabdominal). cUrgency refers to any surgical procedure for rectal prolapse performed on a nonelective basis. ASA: American society of anesthesiology; BMI: body mass index; OR: operating room; IQR: interquartile range; SD: standard deviation. | |||
| Age (year), mean (SD) | 72.0 (12.1) | 68.5 (9.7) | 0.233 |
| Male | 8 (24.2) | 3 (12.0) | 0.320 |
| Multimorbiditya | 11 (33.3) | 2 (8.0) | 0.028 |
| Bedridden | 4 (12.1) | 0 (0) | 0.126 |
| ASA III | 17 (51.5) | 9 (36.0) | 0.451 |
| BMIb, mean (SD) | 21.4 (4.0) | 20.6 (3.5) | 0.463 |
| Urgencyc cases | 12 (36.4) | 1 (4.0) | 0.004 |
| OR time (min), mean (SD) | 52.3 (33.0) | 77.4 (35.1) | 0.007 |
| Blood loss (mL), median (IQR) | 50 (0, 100) | 50 (10, 100) | 0.818 |
| Follow-up time (months), mean (SD) | 21.2 (32.7) | 28.3 (29.9) | |
| ≥ 1 year follow-up | 18 (54.6) | 16 (64.0) | |
| Outcomes | |||
| Complication | 2 (6.1) | 1 (4.0) | > 0.999 |
| Recurrence | 4 (12.1) | 2 (8.0) | 0.690 |
| Constipation | 9 (27.3) | 8 (32.0) | 0.775 |
| Fecal incontinent | 12 (36.4) | 6 (24.0) | 0.396 |
| Hospital stays (day), median (IQR) | 3 (2, 4) | 4 (3, 6) | 0.037 |
| Outcomes | The study outcomes | Sensitivity analysis | |||||||
|---|---|---|---|---|---|---|---|---|---|
| Full-model (n = 58) | More than 1-year follow-upa | Multimorbid modelb | |||||||
| Risk ratio (95% CI) | SE | P | Risk ratio (95% CI) | SE | P | Risk ratio (95% CI) | SE | P | |
| During analysis, the transabdominal approach was treated as the intervention. The risk ratios should be interpreted accordingly (e.g., a lower risk ratio for recurrence indicates a lower recurrence rate for the transabdominal approach, and vice versa). aMore than 1-year follow-up: 18 transperineal vs. 16 transabdominal repairs. bMultimorbid model: replacing the American Society of Anesthesiology III status with the multimorbidity variable (defined as patients having two or more comorbidities or being bedridden) for propensity score calculation. CI: confidence interval; SE: standard error. | |||||||||
| Complication | 0.67 (0.06, 7.65) | 0.83 | 0.749 | 1.18 (0.07, 19.88) | 1.70 | 0.907 | 0.67 (0.06, 7.75) | 0.84 | 0.748 |
| Recurrence | 0.62 (0.11, 3.53) | 0.55 | 0.592 | 0.91 (0.13, 6.46) | 0.91 | 0.927 | 0.56 (0.10, 3.21) | 0.50 | 0.511 |
| Constipation | 0.85 (0.33, 2.19) | 0.41 | 0.733 | 2.24 (0.61, 8.19) | 1.48 | 0.223 | 1.01 (0.37, 2.78) | 0.52 | 0.988 |
| Fecal incontinent | 0.59 (0.23, 1.57) | 0.29 | 0.293 | 0.50 (0.16, 1.60) | 0.30 | 0.244 | 0.44 (0.16, 1.23) | 0.23 | 0.116 |
| Hospital stays (day difference) | 0.02 (-2.09, 2.13) | 1.05 | 0.984 | -0.89 (-5.38, 3.61) | 2.19 | 0.689 | 0.16 (-1.81, 2.14) | 0.99 | 0.869 |