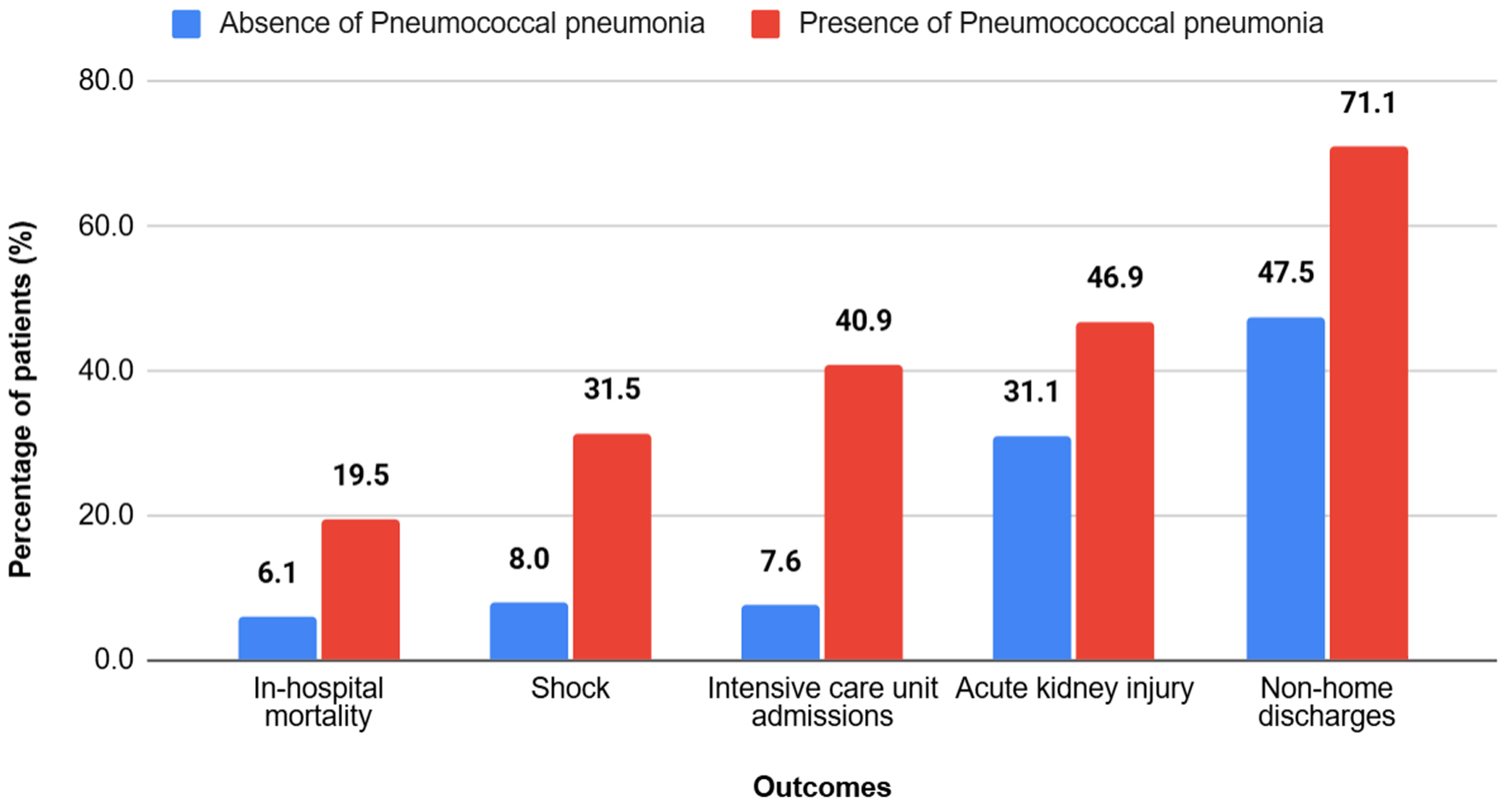
↓ Figure 1. Clinical outcomes among hospitalized patients with cirrhosis, stratified by the presence of pneumococcal pneumonia. Patients with cirrhosis and pneumococcal pneumonia experienced significantly worse clinical outcomes compared with those without pneumococcal pneumonia, including higher rates of in-hospital mortality, shock, intensive care unit admission, acute kidney injury, and non-home discharge (P < 0.001 for all outcomes).