| Gastroenterology Research, ISSN 1918-2805 print, 1918-2813 online, Open Access |
| Article copyright, the authors; Journal compilation copyright, Gastroenterol Res and Elmer Press Inc |
| Journal website https://gr.elmerpub.com |
Original Article
Volume 18, Number 1, February 2025, pages 12-22
Trends and Financial Burden of Gastrointestinal Stromal Tumors in the United States: A Comprehensive Analysis of United States Hospitalizations
Sneh Sonaiyaa, j , Raj Patelb, Charmy Parikhc, Dushyant Dahiyad, Karan Yagnike, Nicolas Alonso Barnechea Alvaradoa, Chun-Han Loa, Kenneth Chowf, Abbas Ali Hussaina, Anushri Parikhg, Pranav Patelh, Babu P. Mohani
aDepartment of Internal Medicine, Kirk Kerkorian School of Medicine at UNLV, University of Nevada Las Vegas, Las Vegas, NV 89102, USA
bDepartment of Internal Medicine, St Mary Medical Center, Langhorne, PA 19047, USA
cDepartment of Internal Medicine, Mercy Catholic Medical Center, Darby, PA 19023, USA
dDepartment of Gastroenterology and Hepatology, The University of Kansas School of Medicine, Kansas City, KS 66103, USA
eDepartment of Internal Medicine, Monmouth Medical Center, Long Branch, NJ 07740, USA
fDepartment of Gastroenterology and Hepatology, Kirk Kerkorian School of Medicine at UNLV, University of Nevada Las Vegas, Las Vegas, NV 89102, USA
gDepartment of Internal Medicine, Baroda Medical College, Vadodara, GJ 390001, India
hDepartment of Gastroenterology and Hepatology, Geisinger Health, Danville, PA 17822, USA
iOrlando Gastroenterology PA, Orlando, FL 32835, USA
jCorresponding Author: Sneh Sonaiya, Department of Internal Medicine, Kirk Kerkorian School of Medicine at UNLV, University of Nevada Las Vegas, Las Vegas, NV 89102, USA
Manuscript submitted December 12, 2024, accepted January 27, 2025, published online February 6, 2025
Short title: Trends of GIST Hospitalizations in the USA
doi: https://doi.org/10.14740/gr2009
| Abstract | ▴Top |
Background: Gastrointestinal stromal tumors (GISTs) are associated with a substantial economic burden to the healthcare system despite their relatively low incidence and prevalence compared to other more common malignancies. This study aimed to evaluate trends in GIST-related hospitalizations, inpatient mortality, and the financial burden of GISTs in the United States.
Methods: The National Inpatient Sample (NIS) database from 2016 to 2020 was used to identify adult hospitalizations (age > 18 years) with a primary diagnosis of GIST. A multivariate logistic regression along with Chi-square and t-tests was performed using SAS 9.4 software to analyze inpatient GIST-associated mortality, inflation-adjusted total hospital charge (THC), and length of stay (LOS) during the study period.
Results: The study analyzed 48,690 hospitalizations (49.2% female, mean age 64.2 years, 38.2% elective admissions) with a primary diagnosis of GIST between 2016 and 2020. Annual GIST-related hospitalizations increased from 2,645 in 2016 to 11,565 in 2020 (P = 0.1208). The most common tumor location was stomach (48.5%), followed by small intestine (18.7%), large intestine (3.6%), and rectum (1.6%). There was a non-significant reduction in inpatient mortality from 4.16% in 2016 to 3.29% in 2020 (P = 0.807). Overall, 36.2% of patients had THC between $10,000 and $20,000 (36.5% in 2016 vs. 34.7% in 2020, P = 0.0001), and 9.8% of patients had a THC > $40,000 (8.3% in 2016 vs. 12.6% in 2020, P = 0.0001). Furthermore, 61.5% of patients had LOS of fewer than 5 days (59.16% in 2016 vs. 61.39% by 2020, P = 0.0001), and 38.5% had LOS of 5 days or more (40.84% in 2016 vs. 38.61% in 2020, P = 0.0001). The proportion of GISTs treated with endoscopic resection has remained stable with 13.02% in 2016 and 13.01% in 2020 (P = 0.08). Additionally, the proportion of surgical excisions decreased from 26.8% in 2016 to 21.4% in 2020 with a statistically significant trend (P = 0.004).
Conclusions: GIST-related inpatient mortality between 2016 and 2020 has remained stable, and endoscopic and surgical interventions have become more common for the management of GISTs. This has been accompanied by a significant rise in overall inflation-adjusted hospitalization costs in the study period. These findings highlight the need for continued optimization of care and resource allocation for GIST management.
Keywords: Gastrointestinal stromal tumors; Epidemiology; Outcomes; Inpatient mortality; Total hospital charge; Length of stay
| Introduction | ▴Top |
Gastrointestinal stromal tumors (GISTs) are the most common mesenchymal tumor of the gastrointestinal (GI) tract, with an annual global incidence ranging from 7 to 20 cases per million adults and a prevalence of 129 per million adults [1-5]. Although GISTs account for less than 1% of all GI tumors, their clinical and economic burden is disproportionately high, reflecting a substantial impact despite their relatively lower incidence compared to more common malignancies such as adenocarcinoma [5-7]. The most common sites for GISTs are the stomach and small intestine [8, 9]. Treatment options include endoscopic or surgical resection for non-metastatic disease and tyrosine kinase inhibitors (TKIs) such as imatinib for advanced and metastatic GIST. The prognosis for GIST varies significantly based on disease stage and tumor location. The 5-year survival rate for localized GIST is 95%, but it decreases to 52% for cases with distant metastases, with a cumulative 5-year disease-specific survival (DSS) estimated at 82% [10, 11]. The healthcare costs associated with GISTs are significant, with cumulative 5-year costs for patients without recurrence estimated at $83,400, while recurrence costs exceed $100,000 over the same period [6].
Historically, a noticeable increase in the incidence of GISTs was reported from 2000 to 2005 attributable to the classification of sarcomas as GISTs [12, 13]. Recent studies have suggested that GISTs located outside the stomach and small bowel, among other factors such as tumor size greater than 5 cm, high histologic grade, age over 60, and the presence of distant metastases, have been associated with poorer outcomes. Conversely, factors such as female sex and undergoing primary surgery were associated with improved overall survival [12]. A 2009 National Inpatient Sample (NIS)-based study using 1 year of hospitalization data showed that GIST patients experience a greater inpatient burden, including longer hospital stays, higher total charges, and increased mortality, compared to patients without GISTs [7].
Despite the significant economic burden and healthcare utilization associated with GISTs, there is a notable paucity of recent data on its trends and outcomes, particularly in the inpatient setting. This study aimed to analyze trends and outcomes of GIST in the United States using the NIS from 2016 to 2020. Hence, in this study, we use the NIS database from 2016 to 2020 to assess hospitalization characteristics, inpatient mortality, and the burden of GISTs on the US Healthcare System. Additionally, we also attempt to identify trends in hospitalizations and healthcare utilization for GIST over this 5-year period.
| Materials and Methods | ▴Top |
Study design and data source
This was a retrospective study that utilized the NIS to analyze hospitalizations in the USA 2016 - 2020. For the purposes of this study, the NIS data from 2016 to 2020 were derived using the International Classification of Diseases, Tenth Revision, Clinical Modification/Procedure Coding System (ICS-10 CM/PCS).
Study population and outcome measures
This study included all adult (≥ 18 years) hospitalizations with a primary diagnosis of GIST from 2016 to 2020. ICD-10 code C49.A (C49.A0, C49.A1, C49.A2, C49.A3, C49.A4, C49.A5, C49.A9) was used for the study.
Outcome measures included GIST-related hospitalization trends, inpatient mortality, and the disease’s financial and hospitalization burden in terms of length of hospital stay (LOS) and total hospital charge (THC). A retrospective multivariate analysis was performed using SAS 9.4 software to analyze inpatient GIST-associated mortality, THC, and LOS during the study period. We obtained the THC using the Healthcare Cost and Utilization Project (HCUP) cost-to-charge ratio (CCR) and adjusted THC for inflation using the Agency for Healthcare Research and Quality (AHRQ) Medical Expenditure Panel Survey (MEPS) 2020 index for inpatient hospital care as a reference [14, 15].
Statistical analysis
All statistical analysis was conducted using SAS 9.4 software (SAS Institute, Cary, NC, USA). Weighted samples were used and descriptive statistics were calculated to determine patient demographics, hospitalization characteristics, and clinical parameters. Descriptive statistics were used to characterize the study population, and Chi-square and t-tests were conducted to assess differences in categorical and continuous variables, respectively. Trends over time were analyzed using Chi-square tests for trend or t-tests, as appropriate. Baseline characteristics included age, sex, race, insurance type, mean household income quartiles, and hospital characteristics based on location and teaching status. THC values were adjusted for inflation using the AHRQ MEPS 2020 index. Two-sided P-values with a significance threshold of 0.05 were used for all statistical tests and analyses were conducted as per HCUP guidelines for the NIS database.
Ethical considerations
The NIS database is de-identified and does not include any patient or hospital-specific identifiers. Hence, our study is exempt from the Institutional Review Board (IRB) approval in accordance with the guidelines established by our institutional IRB for the analysis of HCUP-NIS database study and this study was conducted in compliance with the ethical standards of the responsible institution on human subjects as well as with the Helsinki Declaration.
Data availability statement
The NIS is a large publicly available database in the United States with data on over seven million hospital stays annually along with de-identified information on patient demographics, diagnoses, and hospitalization characteristics [16]. As a component of the HCUP, the NIS uses stratified sampling to generate an all-payer dataset. The NIS collects weighted data on over 35 million hospital admissions per year. Key data like patient demographics, hospital characteristics (including size and location), the primary discharge diagnosis, and procedures carried out during hospital stays are included in this de-identified database that is accessible to the public.
| Results | ▴Top |
Hospitalization characteristics
The study analyzed 48,690 hospitalizations (38.2% elective admissions) with the primary diagnosis of GIST for admission from 2016 to 2020 (Table 1). There was an increase in the annual total number of hospitalizations from GIST in the USA from 2,645 in 2016 to 11,565 in 2020 without a statistically significant trend (P = 0.1208) as demonstrated in Figure 1. Females made up 49.2% of the study cohort. The mean age for these patients decreased from 66.5 years in 2016 to 64.2 years in 2020. The age group 65 - 84 years comprised the highest proportion (50.1%) of the patients followed by 45 - 64 years (34.3%) and > 84 years (8.8%). In terms of racial distribution, the majority of patients were White (58.5%), followed by Black (21.1%), Hispanic (8.3%), Asian or Pacific Islander (5.7%), and Native American (0.3%).
 Click to view | Table 1. Baseline Characteristics of GIST Hospitalizations From NIS 2016 - 2020 |
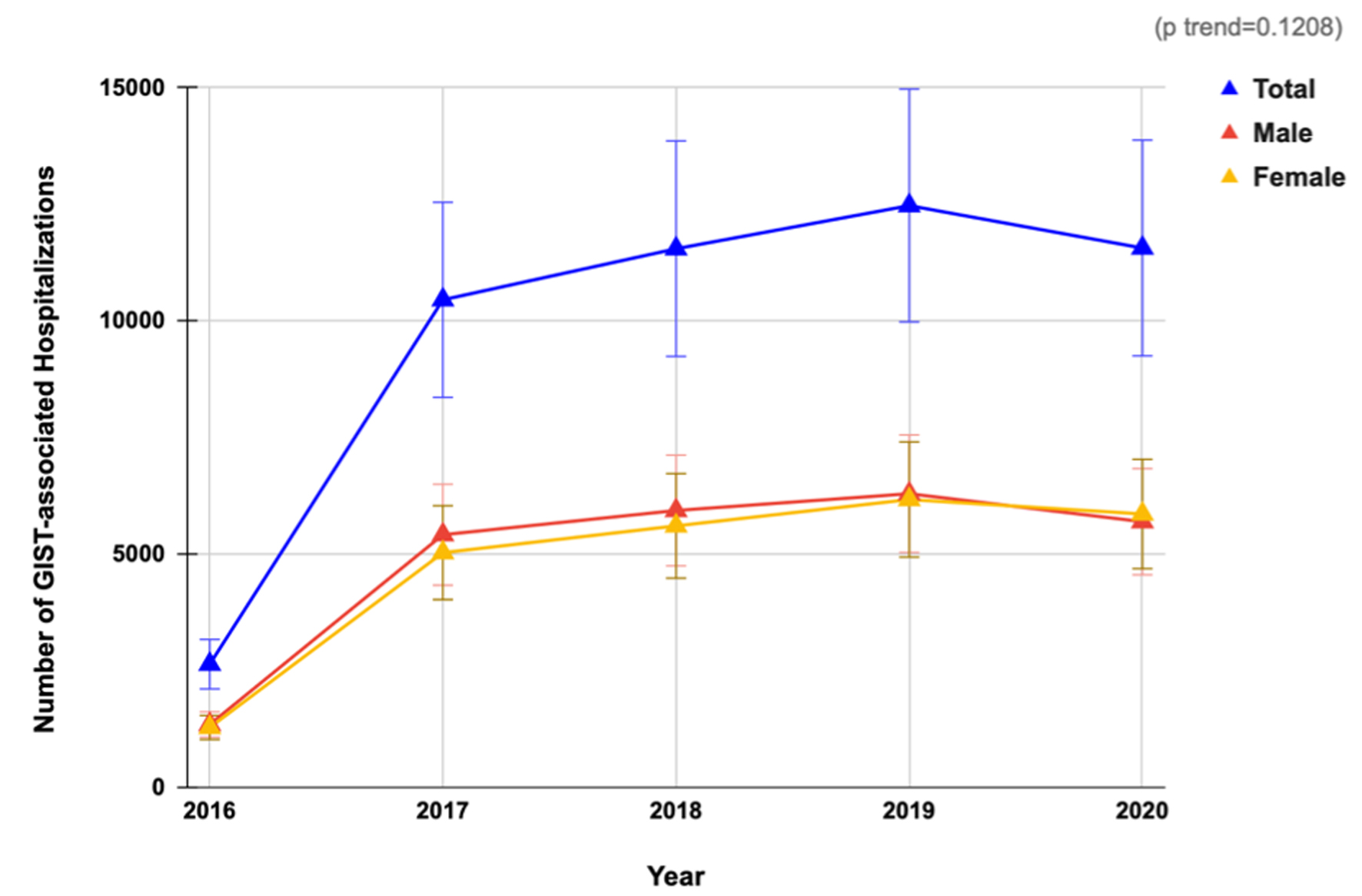 Click for large image | Figure 1. Annual trends in hospitalizations for gastrointestinal stromal tumors: analysis of the National Inpatient Sample 2016 - 2020. |
Regional distribution
In terms of hospital regions, the number of GIST-related hospitalizations was highest in hospitals in the Southern region (36.4%) followed by the West (21.9%), Midwest (21.4%), and Northeast (20.3%) (Fig. 2). Urban teaching hospitals accounted for the majority of cases (82.7%). The proportion of GIST-related hospitalizations across different geographical regions was relatively similar from 2016 to 2020 (Table 1).
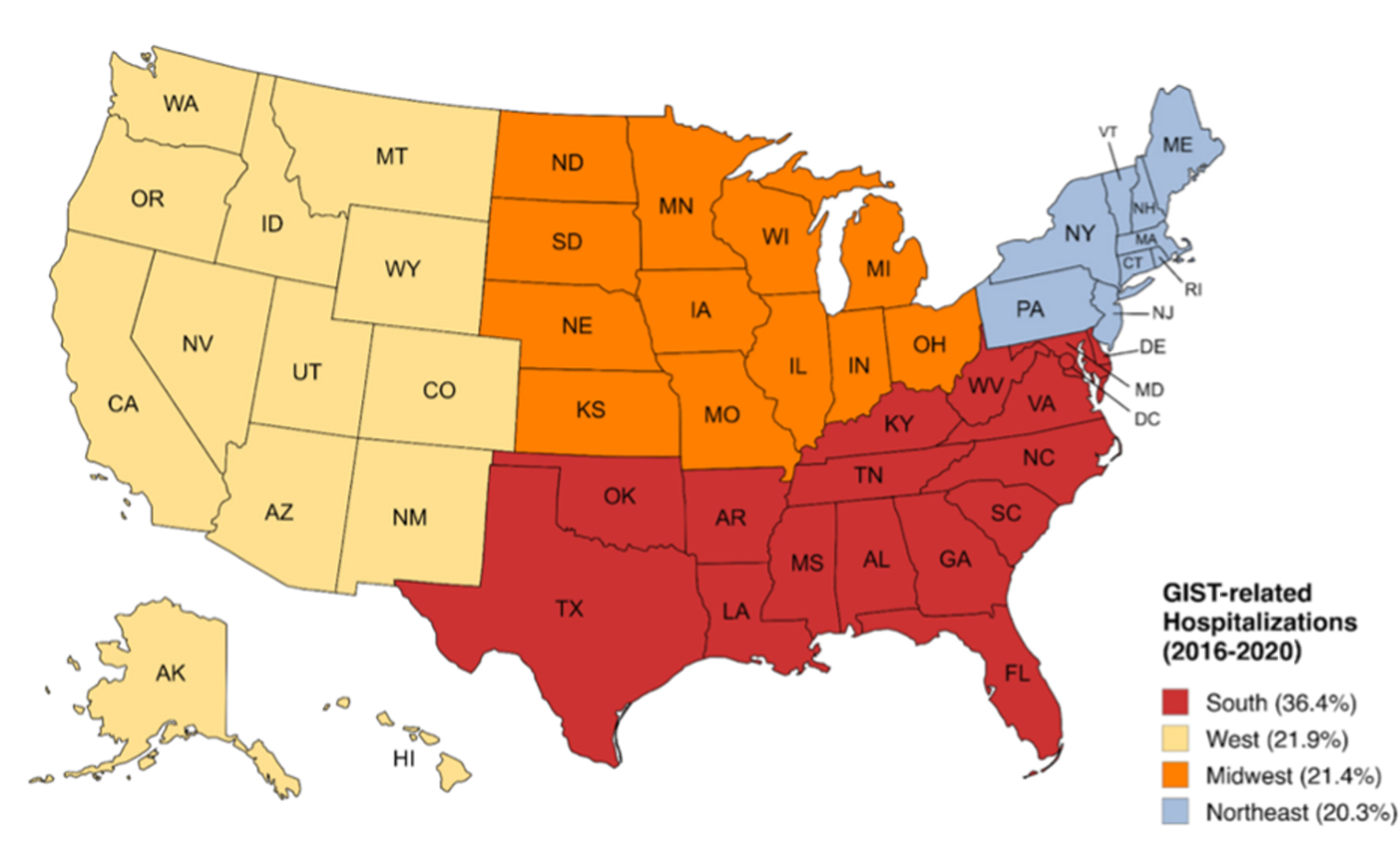 Click for large image | Figure 2. Distribution of gastrointestinal stromal tumor-related hospitalizations based on hospital location in the United States (2016 - 2020): analysis of the National Inpatient Sample 2016 - 2020. |
Clinical outcomes
The most common GIST location was the stomach (48.5%), followed by the small intestine (18.7%), large intestine (3.6%), rectum (1.6%), and unspecified sites (24.1%) (Fig. 3). Between 2016 and 2020, the inpatient mortality rate for patients with hospitalization from GISTs in the USA was 4.16% in 2016 vs. 3.29% in 2020, without a statistically significant trend from 2016 to 2020 (P = 0.807) (Fig. 4). Overall, 36.2% of patients had a THC between $10,000 and $20,000 (36.5% in 2016 vs. 34.7% in 2020, P < 0.0001), and 9.8% of patients had a THC greater than $40,000 (8.3% in 2016 vs. 12.6% in 2020, P < 0.0001) (Table 2). Mean inflation-adjusted THC increased from $20,242 in 2016 to $22,905 in 2020 (P < 0.0001). Additionally, 61.5% of GIST patients had a total LOS of fewer than 5 days (59.16% in 2016 vs. 61.39% by 2020, P = 0.0001), and 38.5% had an LOS of 5 days or more (40.84% in 2016 to 38.61% in 2020, P = 0.0001) (Fig. 5).
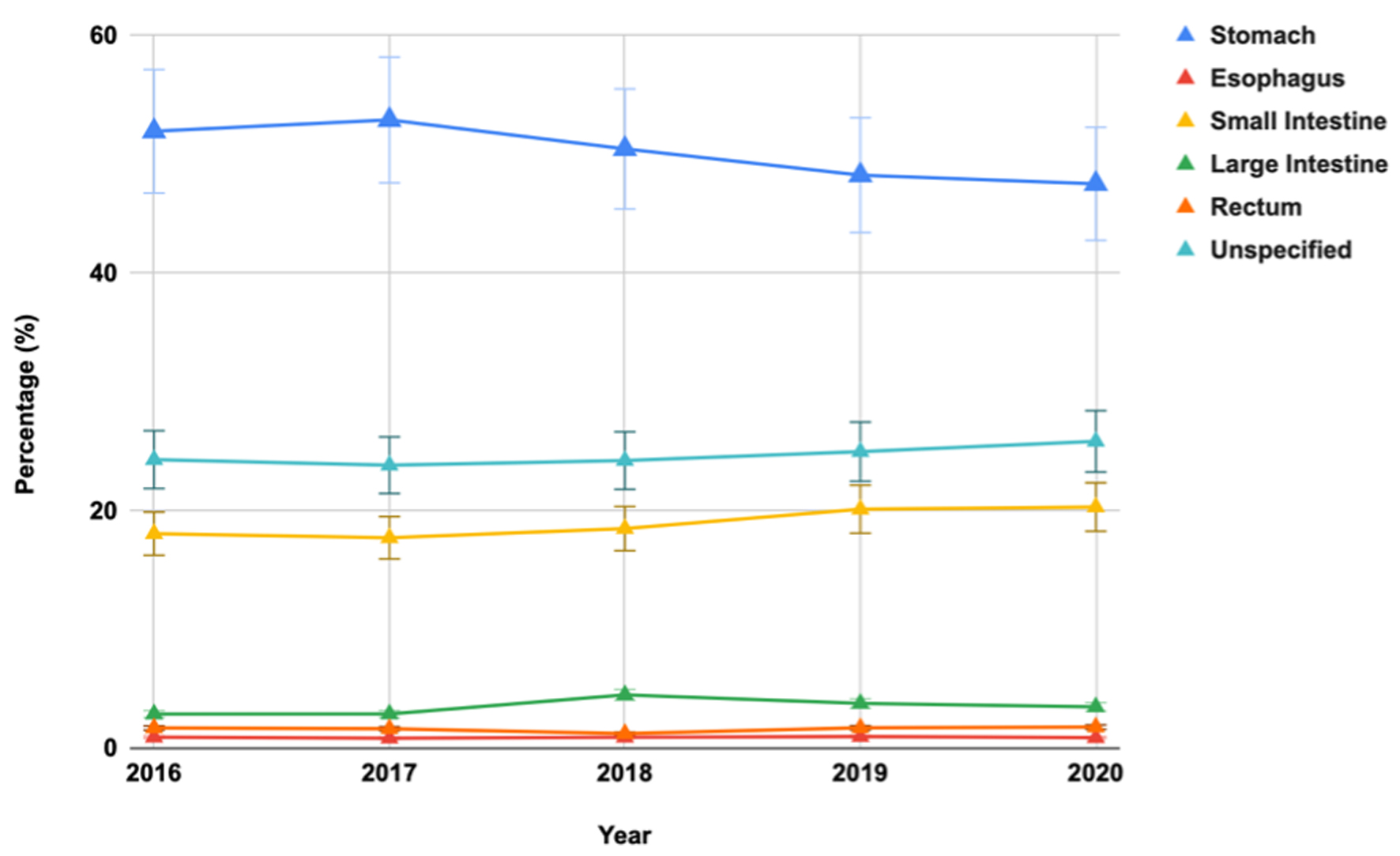 Click for large image | Figure 3. Annual trends in percentage distribution of gastrointestinal stromal tumors based on tumor location: analysis of the National Inpatient Sample 2016 - 2020. |
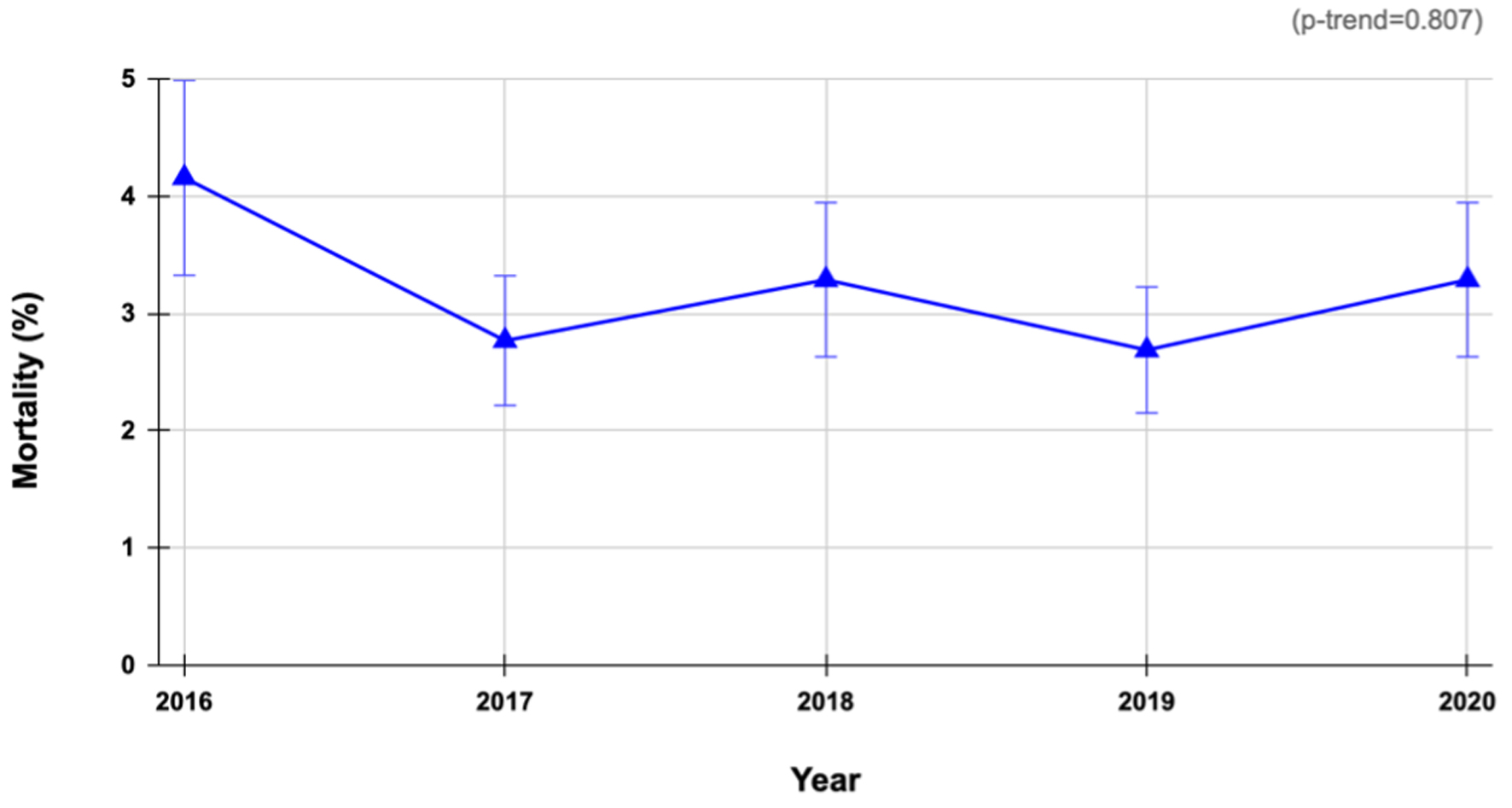 Click for large image | Figure 4. Annual trends in inpatient mortality for gastrointestinal stromal tumors: analysis of the National Inpatient Sample 2016 - 2020. |
 Click to view | Table 2. Annual Trends in Mortality, Tumor Location, Hospital Stay, and Treatment Costs for GISTs From NIS 2016 - 2020 |
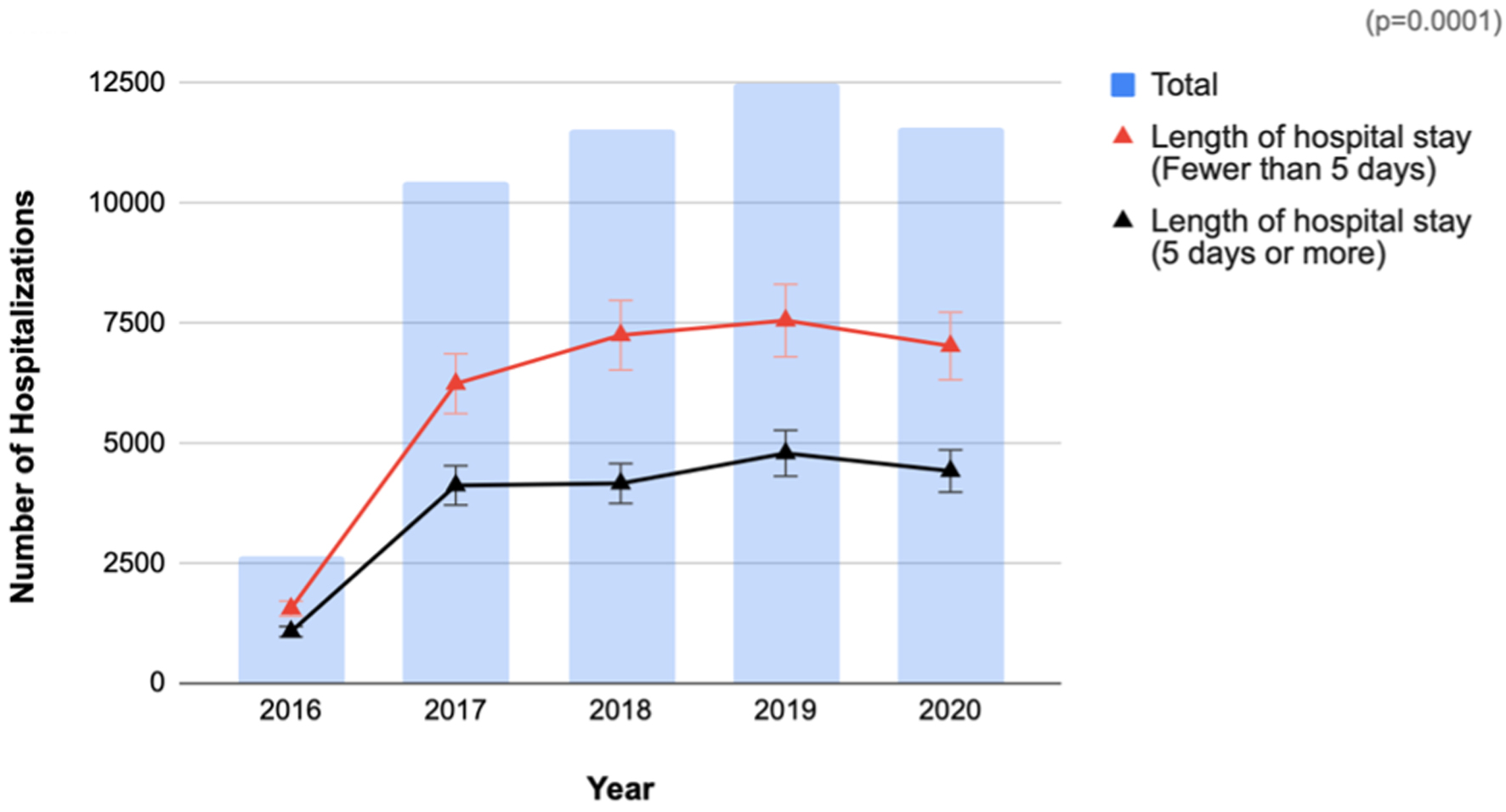 Click for large image | Figure 5. Annual trends in length of hospital stay for gastrointestinal stromal tumors: analysis of the National Inpatient Sample 2016 - 2020. |
Between 2016 and 2020, a total of 1,140 endoscopic excisions, 2,209 surgical excisions, and 489 surgical resections were performed for GIST (Table 3). The proportion of inpatient endoscopic excisions for GISTs has remained stable from 13.02% in 2016 to 13.01% in 2020 without a statistically significant P-trend (P = 0.08). The proportion of surgical resections increased from 3.96% in 2016 to 5.66% in 2020 without a statistically significant P-trend (P = 0.16). Additionally, the proportion of surgical excisions decreased from 26.8% in 2016 to 21.4% in 2020 with a statistically significant trend (P = 0.004) (Table 3).
 Click to view | Table 3. Trends in Endoscopic and Surgical Interventions for GISTs From NIS 2016 - 2020 |
| Discussion | ▴Top |
Overview
In this study of hospitalized patients with GIST, we analyzed trends in hospitalizations, patient demographics, tumor locations, clinical outcomes, LOS, and treatment costs between 2016 and 2020. Our findings demonstrated an overall increase in GIST-related hospitalizations over the study period without a statistically significant trend, with the majority of cases occurring in the 65 - 84 age group and an almost equal gender distribution. The stomach was the most common tumor site, followed by the small intestine. Although there was a non-statistically significant reduction in inpatient mortality, there was a significant increase in inflation-adjusted THCs, with a greater proportion of patients incurring charges above $40,000 by 2020. The LOS for most patients was fewer than 5 days, with a significant increase in this category during the study period. Notably, the proportion of endoscopic excisions remained stable, whereas the proportion of surgical excisions decreased significantly.
Hospitalization characteristics
The study of trends in GIST-associated hospitalizations remains limited. The population-based study from the Netherlands Cancer Registry shows that the incidence of non-metastatic GIST increased from 3.1 per million person-years in 2001 to 7.0 per million person-years in 2012 [17]. A systemic review of 29 studies across 19 countries by Soreide et al reported the most common overall incidence rates to be between 10 and 15 cases per million population per year. The highest rates were observed in regions such as China (Hong Kong and Shanghai), Taiwan, Korea, and Norway, with incidences ranging from 19 to 22 cases per million population per year [3]. In contrast, the incidence in North America is reported to be lower, with rates in the United States and Canada in most studies typically ranging from 7 to 8 cases per million population per year [3, 18, 19].
Our study demonstrates an increase in GIST-related hospitalizations from 2,645 in 2016 to 11,565 in 2020, although this trend was not statistically significant (Table 1). Our findings were consistent with the population-based studies by Khan et al (2022) and Alvarez et al showing an overall increase in GIST cases since 2000 [12, 20]. Since the National Comprehensive Cancer Network (NCCN) guidelines for initial diagnostic workup for GIST have remained fairly unchanged over the years, the broader availability of advanced diagnostic imaging, particularly at urban teaching hospitals, may help explain the rise in GIST-related hospitalizations observed in our study [21, 22].
Regarding patient characteristics, hospitalizations were most common among patients aged 65 - 84 years, consistent with findings from prior studies [9, 12]. In our study, patients from the 0-25th percentile income quartile represented a slightly higher proportion of hospitalizations. The overall proportion of GIST-related hospitalizations during the study period have remained stable across different income quartiles. Additionally, we observed a rising proportion of GIST-related hospitalizations occurring in urban teaching hospitals, which increased from 79.6% in 2016 to 82.7% in 2020. This shift may have contributed to the overall rising trend in hospitalizations, as urban teaching hospitals tend to have more advanced diagnostic and treatment capabilities.
Common comorbidities noted among GIST patients were hypertension, diabetes mellitus, and chronic pulmonary disease (Table 1). Additionally, metastatic cancer was noted in 15.7% of hospitalizations. The predominance of non-elective admissions (61.7%) further indicates that many hospitalizations were driven by urgent or emergent needs. The stomach and small intestine were identified as the primary sites for GISTs, collectively accounting for nearly two-thirds of cases over the study period. This distribution aligns with existing literature, which reports that approximately 50-60% of GISTs originate in the stomach and 20-30% in the small intestine [3, 12]. The majority of hospitalizations in our study were among White, followed by Black, Hispanic, and Asian or Pacific Islander populations. Interestingly, previous studies have suggested that GIST incidence may be higher in African Americans compared to other ethnic groups, highlighting potential racial differences in disease prevalence or healthcare utilization patterns [23, 24]. Our study results for the year 2020 should be interpreted with caution as the COVID-19 pandemic may have disrupted typical hospitalization patterns [25].
Inpatient mortality
Several studies have reported that extra-gastric GISTs have higher malignant potential and are associated with poorer outcomes [26, 27]. The population-based study by Khan et al reported that GISTs located outside the stomach and small bowel were associated with poorer outcomes [12]. Another population-based study reported the 5-year GIST-specific mortality to be 12.9% [28].
Our study showed an overall annual mortality of 4.16% in 2016 to 3.29% in 2020, without a statistically significant P-trend. For comparison, a previous study by Datar et al based on the analysis of the NIS database in 2009 showed a mortality rate of 4.62% in patients with GISTs [7]. The lower observed mortality in our study compared to previous studies may stem from early diagnosis, improved management, and better follow-up for GIST. Imatinib is a TKI that was first approved by the US Food and Drug Administration (FDA) for GISTs in 2002. In recent years, several newer TKIs have also received FDA approval, further expanding the therapeutic options available for GIST management, and the slight reduction in inpatient mortality noted from 2016 to 2020 in our study could be from the improved therapeutic options for GISTs [29, 30]. It is important to note that the inpatient mortality in patients hospitalized with a diagnosis of GIST may be different from mortality secondary to GISTs in the general population. Further research is needed to assess GIST-related mortality based on clinical staging and other risk factors to better understand prognostic factors that could guide therapeutic interventions.
Burden of GIST on the US Healthcare System
GISTs impose a substantial economic burden on the healthcare system, as evidenced by the significant upward trend in hospital charges. Our study demonstrated that the mean inflation-adjusted THC increased from $20,242 in 2016 to $22,905 in 2020. Additionally, the proportion of patients with a THC exceeding $40,000 increased significantly, from 8.3% in 2016 to 12.6% in 2020.
A retrospective study estimated that GIST-attributable cost in the first year after surgical resection was approximately $23,300 and the economic burden associated with GIST increases nearly twice upon the recurrence of GIST [6]. Comparing our results to prior studies, Datar et al reported a mean THC of $49,429 for GIST-related hospitalizations based on 2009 NIS data, which appears higher than the total charges observed in our study. Several factors could explain this difference. Firstly, advancements in diagnostic and therapeutic technologies may have contributed to the shortened LOS in recent years, thereby reducing inpatient costs. For instance, the LOS in our study ranged from 4.87 to 5.23 days during the study period, significantly lower than the mean LOS of 6.72 days reported by Datar et al. Additionally, nearly 61.5% of the total hospitalizations in our study had an LOS of fewer than 5 days, and the longer hospital stays (5 days or more) decreased from 40.84% to 38.61% during our study period.
Additionally, our study demonstrated a statistically significant downward trend in the proportion of surgical excisions for GISTs from 26.8% to 21.4% in the study period, whereas the proportion of inpatient endoscopic excisions for GISTs has remained stable in the study period (Table 3). The relatively low proportions of inpatient endoscopic or surgical excisions are likely attributable to the increasing management of GISTs in outpatient settings. These settings provide several advantages, including shorter recovery times, reduced costs, and minimized exposure to hospital-associated risks, which collectively decrease the necessity for inpatient procedures [31].
Moreover, studies have highlighted the significant costs associated with TKIs for GISTs [32, 33]. Recent studies have suggested that the introduction of TKIs has likely allowed for quicker transitions from inpatient care to outpatient management, reducing the necessity of extended hospital stays [34]. As a result, inpatient THC may not fully capture the true treatment costs associated with GISTs. The trend toward shorter hospital stays, minimally invasive techniques, and broader adoption of outpatient follow-up for GISTs may contribute to the economic burden noted in our study. Future studies should incorporate outpatient costs to evaluate the cumulative financial impact of GIST treatment across care settings.
Strengths and limitations
This study has several key strengths and limitations. A significant strength lies in the study population, NIS, which is one of the largest publicly available databases in the USA, containing data on more than seven million hospital stays. This dataset includes inpatient admissions from hospitals across the country, making the findings broadly applicable to healthcare institutions nationwide. Consequently, the NIS database would be optimal for identifying key trends in GIST-related hospitalizations, mortality, and other clinical outcomes, thereby allowing us to draw meaningful conclusions.
However, there are a few limitations of the study. Firstly, the NIS database does not provide data on the severity of GIST, time to diagnosis, hospital course, or other aspects of treatment for GIST. Furthermore, since this study is retrospective, all the inherent biases of retrospective studies also apply to this study. The hospitalizations recorded in the NIS database are based on the diagnosis of GIST rather than individual patients. Hence, the individuals admitted multiple times for the same diagnosis may have been counted more than once in the dataset. Lastly, since NIS is an administrative dataset and is based on specific codes, the possibility of coding errors cannot be excluded. Despite the limitations, we believe that the large sample size of our study over a 5-year period and comprehensive analysis provide valuable insights into the GIST-related trends and outcomes over the study period.
Conclusion
Our study highlights a notable increase in GIST-related hospitalizations, predominantly among older adults, with the stomach and small intestine remaining the most common tumor sites. While inpatient mortality showed a slight, non-statistically significant decline, there was a marked rise in THCs. The evolving management landscape of GISTs is evident from the shift toward shorter hospital stays, a substantial decrease in surgical excisions, and stable rates of endoscopic interventions. Our study findings provide insights into the changing landscape of GISTs, highlighting the need to optimize diagnostic and therapeutic strategies to mitigate the growing economic burden of GISTs on the healthcare system.
Acknowledgments
The publication fees for this article were supported by the University of Nevada Las Vegas (UNLV) School of Medicine Library Open Article Fund.
Financial Disclosure
The authors have no financial disclosures to declare.
Conflict of Interest
The authors have no conflict of interest to declare.
Informed Consent
Since the NIS lacks patient identifiers, no informed consent is required for the NIS study.
Author Contributions
Sneh Sonaiya: conceptualization, data curation, writing original draft, project administration, visualization; Raj Patel: conceptualization, methodology, software, formal analysis, resources, data curation; Charmy Parikh: writing original draft, project administration; Dushyant Dahiya: writing - review and editing, supervision; Karan Yagnik: writing original draft; Nicolas Alonso Barnechea Alvarado: writing - review and editing; Chun-Han Lo: writing - review and editing; Kenneth Chow: writing - review and editing; Abbas Ali Hussain: writing - review and editing; Anushri Parikh: resources, data curation; Pranav Patel: validation, supervision, project administration; Babu P. Mohan: writing - review and editing, supervision, project administration.
Data Availability
We utilized the NIS database from 2016 to 2020 for our analysis. The NIS database is available at: https://hcup-us.ahrq.gov/nisoverview.jsp
Abbreviations
AHRQ: Agency for Healthcare Research and Quality; CCR: cost-to-charge ratio; DSS: disease-specific survival; FDA: Food and Drug Administration; GIST: gastrointestinal stromal tumor; HCUP: Healthcare Cost and Utilization Project; ICS-10 CM/PCS: International Classification of Diseases, Tenth Revision, Clinical Modification/Procedure Coding System; IRB: Institutional Review Board; LOS: length of stay; MEPS: Medical Expenditure Panel Survey; NCCN: National Comprehensive Cancer Network; NIS: National Inpatient Sample; THC: total hospital charge; TKI: tyrosine kinase inhibitor
| References | ▴Top |
- Eisenberg BL, Pipas JM. Gastrointestinal stromal tumor—background, pathology, treatment. Hematol Oncol Clin North Am. 2012;26(6):1239-1259.
doi pubmed - Stamatakos M, Douzinas E, Stefanaki C, Safioleas P, Polyzou E, Levidou G, Safioleas M. Gastrointestinal stromal tumor. World J Surg Oncol. 2009;7:61.
doi pubmed - Soreide K, Sandvik OM, Soreide JA, Giljaca V, Jureckova A, Bulusu VR. Global epidemiology of gastrointestinal stromal tumours (GIST): A systematic review of population-based cohort studies. Cancer Epidemiol. 2016;40:39-46.
doi pubmed - Gupta P, Tewari M, Shukla HS. Gastrointestinal stromal tumor. Surg Oncol. 2008;17(2):129-138.
doi pubmed - Nilsson B, Bumming P, Meis-Kindblom JM, Oden A, Dortok A, Gustavsson B, Sablinska K, et al. Gastrointestinal stromal tumors: the incidence, prevalence, clinical course, and prognostication in the preimatinib mesylate era—a population-based study in western Sweden. Cancer. 2005;103(4):821-829.
doi pubmed - Rubin JL, Sanon M, Taylor DC, Coombs J, Bollu V, Sirulnik L. Epidemiology, survival, and costs of localized gastrointestinal stromal tumors. Int J Gen Med. 2011;4:121-130.
doi pubmed - Datar M, Khanna R. Inpatient burden of gastrointestinal stromal tumors in the United States. J Gastrointest Oncol. 2012;3(4):335-341.
doi pubmed - Aggarwal M, Aggarwal A, Arora S, Rathi AK, Singh K. Demographic and clinicopathological profile of patients of gastrointestinal stromal tumor from a tertiary care center of North India: An observational study. J Cancer Res Ther. 2020;16(Supplement):S104-S109.
doi pubmed - Miettinen M, Lasota J. Gastrointestinal stromal tumors: review on morphology, molecular pathology, prognosis, and differential diagnosis. Arch Pathol Lab Med. 2006;130(10):1466-1478.
doi pubmed - Huang HY, Li CF, Huang WW, Hu TH, Lin CN, Uen YH, Hsiung CY, et al. A modification of NIH consensus criteria to better distinguish the highly lethal subset of primary localized gastrointestinal stromal tumors: a subdivision of the original high-risk group on the basis of outcome. Surgery. 2007;141(6):748-756.
doi pubmed - Survival rates for gastrointestinal stromal tumors | American Cancer Society. https://www.cancer.org/cancer/types/gastrointestinal-stromal-tumor/detection-diagnosis-staging/survival-rates.html. Accessed December 10, 2024.
- Khan J, Ullah A, Waheed A, Karki NR, Adhikari N, Vemavarapu L, Belakhlef S, et al. Gastrointestinal stromal tumors (GIST): a population-based study using the SEEr database, including management and recent advances in targeted therapy. Cancers (Basel). 2022;14(15):3689.
doi pubmed - Perez EA, Livingstone AS, Franceschi D, Rocha-Lima C, Lee DJ, Hodgson N, Jorda M, et al. Current incidence and outcomes of gastrointestinal mesenchymal tumors including gastrointestinal stromal tumors. J Am Coll Surg. 2006;202(4):623-629.
doi pubmed - HCUP Cost-to-Charge Ratio (CCR). 2001 - 2022. Agency for healthcare research and quality, Rockville, MD. https://hcup-us.ahrq.gov/db/ccr/ip-ccr/ip-ccr.jsp. Accessed December 9, 2024.
- Medical expenditure panel survey: hospital inpatient stays. Agency for healthcare research and quality, Rockville, MD. https://meps.ahrq.gov/mepsweb/data_stats/download_data_files_results.jsp?cboDataYear=All&cboDataTypeY=2%2CHousehold+Event+File&buttonYearandDataType=Search&cboPufNumber=All&SearchTitle=Hospital+Inpatient+Stays. Accessed December 10, 2024.
- HCUP National (Nationwide) Inpatient Sample (NIS). Agency for Healthcare Research and Quality, Rockville, MD. https://hcup-us.ahrq.gov/db/nation/nis/nisdbdocumentation.jsp. Accessed December 10, 2024.
- van der Graaf WTA, Tielen R, Bonenkamp JJ, Lemmens V, Verhoeven RHA, de Wilt JHW. Nationwide trends in the incidence and outcome of patients with gastrointestinal stromal tumour in the imatinib era. Br J Surg. 2018;105(8):1020-1027.
doi pubmed - Ma GL, Murphy JD, Martinez ME, Sicklick JK. Epidemiology of gastrointestinal stromal tumors in the era of histology codes: results of a population-based study. Cancer Epidemiol Biomarkers Prev. 2015;24(1):298-302.
doi pubmed - Patel N, Benipal B. Incidence of gastrointestinal stromal tumors in the United States from 2001-2015: a United States cancer statistics analysis of 50 states. Cureus. 2019;11(2):e4120.
doi pubmed - Alvarez CS, Piazuelo MB, Fleitas-Kanonnikoff T, Ruhl J, Perez-Fidalgo JA, Camargo MC. Incidence and survival outcomes of gastrointestinal stromal tumors. JAMA Netw Open. 2024;7(8):e2428828.
doi pubmed - von Mehren M, Kane JM, Riedel RF, Sicklick JK, Pollack SM, Agulnik M, Bui MM, et al. NCCN Guidelines(R) insights: gastrointestinal stromal tumors, Version 2.2022. J Natl Compr Canc Netw. 2022;20(11):1204-1214.
doi pubmed - Demetri GD, von Mehren M, Antonescu CR, DeMatteo RP, Ganjoo KN, Maki RG, Pisters PW, et al. NCCN Task Force report: update on the management of patients with gastrointestinal stromal tumors. J Natl Compr Canc Netw. 2010;8(Suppl_2):S1-41; quiz S42-44.
doi pubmed - Tran T, Davila JA, El-Serag HB. The epidemiology of malignant gastrointestinal stromal tumors: an analysis of 1,458 cases from 1992 to 2000. Am J Gastroenterol. 2005;100(1):162-168.
doi pubmed - Ulanja MB, Rishi M, Beutler BD, Konam KG, Ambika S, Hinojosa T, Djankpa FT, et al. Racial disparity in incidence and survival for gastrointestinal stromal tumors (GISTs): an analysis of SEER database. J Racial Ethn Health Disparities. 2019;6(5):1035-1043.
doi pubmed - Adekunle AD, Rubens M, Sedarous M, Tariq T, Okafor PN. Trends in gastrointestinal disease hospitalizations and outcomes during the first year of the coronavirus pandemic. World J Gastroenterol. 2023;29(4):744-757.
doi pubmed - Yi JH, Park BB, Kang JH, Hwang IG, Shin DB, Sym SJ, Ahn HK, et al. Retrospective analysis of extra-gastrointestinal stromal tumors. World J Gastroenterol. 2015;21(6):1845-1850.
doi pubmed - Zhang H, Liu Q. Prognostic indicators for gastrointestinal stromal tumors: a review. Transl Oncol. 2020;13(10):100812.
doi pubmed - Coe TM, Fero KE, Fanta PT, Mallory RJ, Tang CM, Murphy JD, Sicklick JK. Population-based epidemiology and mortality of small malignant gastrointestinal stromal tumors in the USA. J Gastrointest Surg. 2016;20(6):1132-1140.
doi pubmed - Kumar V, Doros L, Thompson M, Mushti SL, Charlab R, Spehalski EI, Zhao H, et al. FDA approval summary: ripretinib for advanced gastrointestinal stromal tumor. Clin Cancer Res. 2023;29(11):2020-2024.
doi pubmed - Naito Y, Nishida T, Doi T. Current status of and future prospects for the treatment of unresectable or metastatic gastrointestinal stromal tumours. Gastric Cancer. 2023;26(3):339-351.
doi pubmed - Young S, Osman B, Shapiro FE. Safety considerations with the current ambulatory trends: more complicated procedures and more complicated patients. Korean J Anesthesiol. 2023;76(5):400-412.
doi pubmed - Talon B, Calip GS, Lee TA, Sharp LK, Patel P, Touchette DR. Trend in tyrosine kinase inhibitor utilization, price, and out-of-pocket costs in patients with chronic myelogenous leukemia. JCO Oncol Pract. 2021;17(11):e1811-e1820.
doi pubmed - Targeted therapy for gastrointestinal stromal tumors | American Cancer Society. https://www.cancer.org/cancer/types/gastrointestinal-stromal-tumor/treating/targeted-therapy.html. Accessed December 10, 2024.
- Mocellin S, Pasquali S, Campana L, Yuan Y, Gronchi A, Griffiths E, Vohra R, et al. Tyrosine kinase inhibitor therapies for gastrointestinal stromal tumours. Cochrane Database Syst Rev. 2018;2018(2):CD012951.
doi
This article is distributed under the terms of the Creative Commons Attribution Non-Commercial 4.0 International License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited.
Gastroenterology Research is published by Elmer Press Inc.